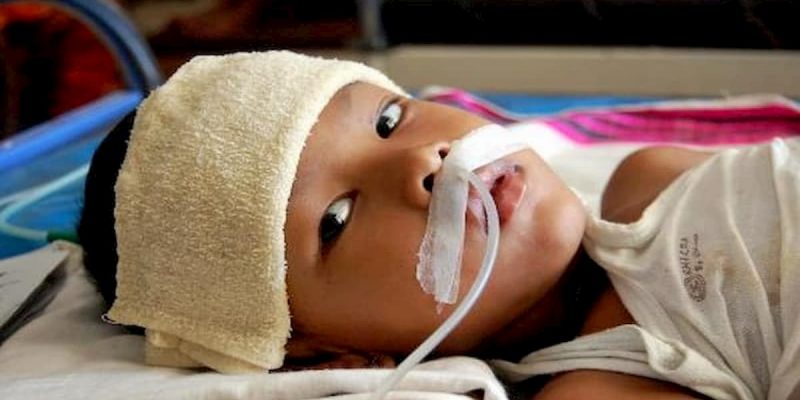
This genetic disorder can occur at any age of people, but the majority of Muscular Dystrophy signs and symptoms occur during childhood.
What is Muscular Dystrophy
Muscular dystrophy is a genetic disorder that weakens the body’s muscles. It’s happening because of incorrect or missing genetic information that prevents the body from making the proteins that needed to build and maintain healthy muscles. This damage and weakness is due to the lack of a protein called dystrophin, which is necessary for normal muscle function. The absence of this protein can cause problems with walking, swallowing, and muscle coordination.

Usually, young boys are more likely to suffer from this disease. Over time, children with this disease will become weakened, loss ability to walk, sit, and lift objects. It can also influence muscles in the lung and hearts. Serious heart and face problem while breathing also can occur.
Types of Muscular Dystrophy
Duchenne Muscular Dystrophy
- The most common form of the illness. Symptoms normally start before a child’s third birthday; they are generally wheelchair-bound by 12 years and die of respiratory failure by their early-to-mid-twenties.
Becker muscular dystrophy
- Similar symptoms to Duchenne but with a later onset and slower progression; death usually occurs in the mid-forties.
Myotonic (Steinert’s disease)
- The myotonic form is the most common adult-onset form. It is characterized by an inability to relax a muscle once it has contracted. The muscles of the face and neck are often affected first. Symptoms also include cataracts, sleepiness, and arrhythmia.
Congenital
- This type can be obvious from birth or before the age of 2 years. It affects girls and boys. Some forms progress slowly whereas others can move swiftly and cause significant impairment.
Facioscapulohumeral (FSHD)
- Onset can be at almost any age but is most commonly seen during teenage years. The muscular weakness often begins in the face and shoulders. People with FSHD may sleep with their eyes slightly open and have trouble fully closing their eyelids. When an individual with FSHD raises their arms, their shoulder blades protrude like wings.
Limb-girdle
- This variant begins in childhood or teenage years and first effects the shoulder and hip muscles. Individuals with the limb-girdle muscular dystrophy might have trouble raising the front part of the foot, making tripping a common problem.
Oculopharyngeal muscular dystrophy
- Onset is between the ages of 40 and 70 years. Eyelids, throat, and face are first affected, followed by the shoulder and pelvis.
How is muscular dystrophy diagnosed?
A number of different tests can help your doctor diagnose a muscular dystrophy. Your doctor can:
- Test your blood for the enzymes released by damaged muscles
- Test your blood for the genetic markers of muscular dystrophy
- Perform an electromyography test on your muscle’s electrical activity using an electrode needle that enters your muscle
- Perform a muscle biopsy to test a sample of your muscle for muscular dystrophy
Muscular Dystrophy signs and symptoms
For most types of this disease, the indications start to show up in childhood or in the teen years. In general, children will show the condition:
- Often falls
- Weak muscles
- Muscle cramp
- Walk on their toes
- Trouble to getting up, climbing stairs, jumping or running
Some others will also have signs like:
- Droopy eyelids
- Heart problems
- Vision problems
- Trouble breathing or swallowing
- A curved spine or called scoliosis
- Weakness in the muscles of the face
How is muscular dystrophy treated?
There’s currently no cure for muscular dystrophy, but treatments can help manage the muscular dystrophy signs and symptoms and slow the progression of the disease. Treatments for this disease would be depending on each Muscular Dystrophy signs and symptoms.
Treatment options include:
- corticosteroid drugs, which help strengthen your muscles and slow muscle deterioration
- assisted ventilation if respiratory muscles are affected
- medication for heart problems
- surgery to help correct the shortening of your muscles
- surgery to repair cataracts
- surgery to treat scoliosis
- surgery to treat cardiac problems
Physical therapy
A range of motion and stretching exercises can help combat the inevitable inward movement of the limbs as muscles and tendons shorten. Limbs tend to become fixed in position, and these types of activities can help keep them mobile for longer. Standard low-impact aerobic exercises such as walking, and swimming can also help slow the disease’s progression.
The progressive Muscular Dystrophy signs and symptoms include:
- Trouble walking. Some people with muscular dystrophy eventually need to use a wheelchair.
- Shortening of muscles or tendons around joints (contractures). Contractures can further limit mobility.
- Breathing problems. Progressive weakness can affect the muscles associated with breathing. People with muscular dystrophy may eventually need to use a breathing assistance device (ventilator), initially at night but possibly also during the day.
- Curved spine (scoliosis). Weakened muscles may be unable to hold the spine straight.
- Heart problems. Muscular dystrophy can reduce the efficiency of the heart muscle.
- Swallowing problems. If the muscles involved with swallowing are affected, nutritional problems and aspiration pneumonia may develop. Feeding tubes may be an option.
Get Insurance Financial Advice
Financial Security – It is There When Needed
Levine can help you to protect yourself and the future of your loved ones. Get immediate financial security. Don’t touch your savings. Let insurance provide it.
She can help provide financial security in times of hardship and will be able to ease the financial burden of your dependents in your absence.
Contact our AIA INSURANCE AGENT LEVINE LEE to get in touch with us and start your personal coverage, group coverage or choose your plan now. Get covered correctly. Be advised correctly. Call Levine Lee (+6012-684 0948) today to be advised on the best insurance protection personalized for you. Or send us the form below on your interest.

At Red Cover Life Planning, we emphasize our people- helping them grow, expanding their abilities, and discovering new opportunities. Join us now to be part of our team and story.